Endoscopic third ventriculostomy, an operation where a small hole is made in the floor of the third ventricle of the brain through the use of an endoscope, was first performed back in 1923, where it remains an option for the treatment of hydrocephalus. Although perhaps less popular since the advent of shunt systems back in the 1960s, shunts may not necessarily be suitable for certain patients, and so in select cases, a growing number of surgeons are recommending ETV.
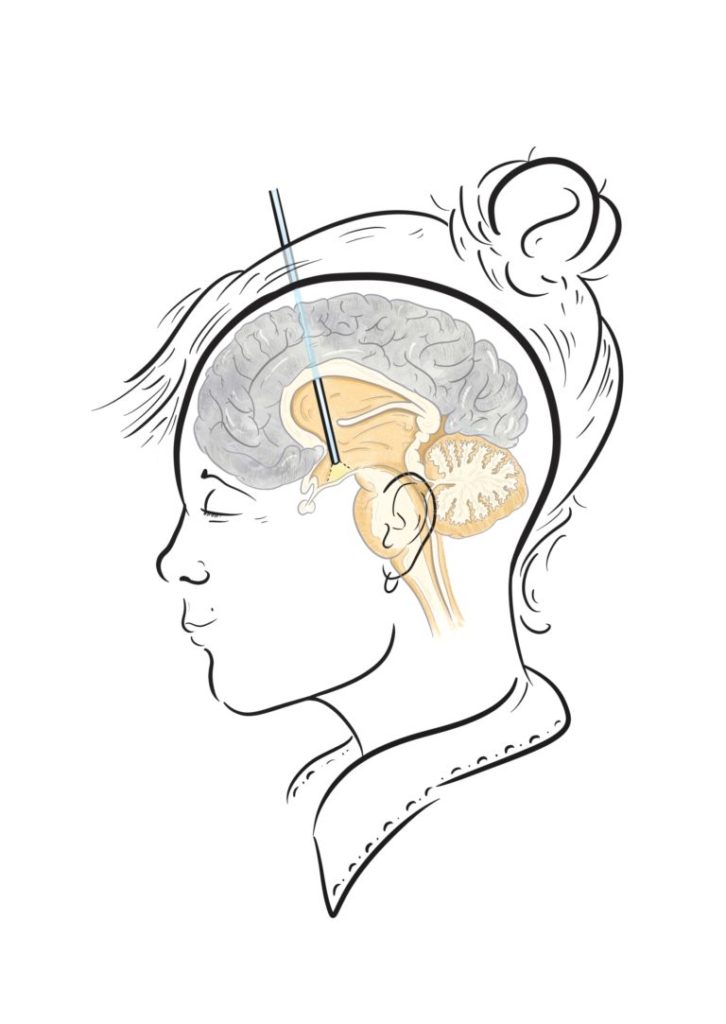
What is ETV and how does it work?
In ETV, a technology called endoscopy or neuroendoscopy is used – put simply, this involves making a small incision and burr hole, the size of a 5p coin, in the top of the head before passing a small scope into the third ventricle, giving your neurosurgeon a view of the ventricular system. A balloon catheter is then placed through a channel in the endoscope – the surgeon can then precisely make a small hole with the tip before inflating the balloon in this hole to widen it, allowing the cerebrospinal fluid to leave the ventricle and circumvent any obstructions.
What are the advantages?
In this way ETV possesses a number of varying advantages and disadvantages in comparison to other treatments and interventions for the management of hydrocephalus.
Advantages include:
- Arguably the main advantage of ETVs, there is less risk of infection as no foreign objects such as shunts or valves are implanted into the body.
- Lower long term complication rate in comparison to the shunt procedure.
- Less incisions in comparison to the shunt procedure.
What are the disadvantages?
- ETV can carry a risk of more serious complications like sudden pathway closure
- Surgeons need to be highly selective of which patients they can do an ETV on.
Are there any risks?
As with all operations, ETV carries some risk. The below are potential complications that may occur:
- Injury to neural structures (short term memory loss)
- Sudden pathway closure – this most commonly happens at around 6 months and can be sudden and life-threatening
- Haemorrhage
- Infection
- Haematoma
- CSF leak
Credits

Stasa Tumpa
Brainbook Ambassador programme deputy lead
Illustrations
Merlin
Medical Illustrator
Merlin is an award-winning Medical Illustrator, Writer, Educator and Director of ‘Drawn to Medicine’. She strives to visualise information in a way that makes it universally accessible, educational and engaging for both clinicians, patients and the general public.
Follow her on Twitter: @merlin_draws

Leave a Reply